Why Is a Baby in Breech Uncomfortable to Carry?
| Breech birth | |
|---|---|
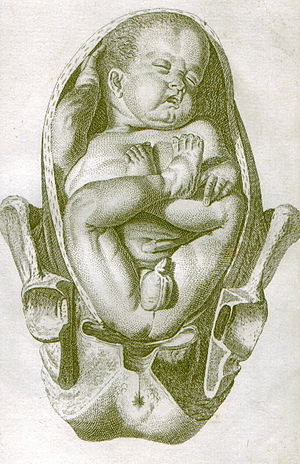 | |
| Drawing of a frank breech from 1754 by William Smellie | |
| Specialty | Obstetrics, midwifery |
A breech birth is when a baby is built-in bottom first instead of caput first, equally is normal.[1] Effectually 3–five% of significant women at term (37–40 weeks pregnant) take a breech baby.[2] Due to their higher than average rate of possible complications for the baby, breech births are by and large considered higher risk.[3] Breech births also occur in many other mammals such every bit dogs and horses, come across veterinary obstetrics.
Virtually babies in the breech position are delivered via caesarean section because it is seen as safer than being born vaginally.[2] Doctors and midwives in the developing world often lack many of the skills required to safely aid women giving birth to a breech infant vaginally.[2] Also, delivering all breech babies by caesarean section in developing countries is difficult to implement as there are not e'er resource available to provide this service.[4] OB-GYNs do not recommend home births if a breech birth is expected, even when attended by a medical professional person.[5]
Cause [edit]
With regard to the fetal presentation during pregnancy, 3 periods have been distinguished.[six]
During the first period, which lasts until the 24th gestational week, the incidence of a longitudinal lie increases, with equal proportions of breech or cephalic presentations from this prevarication. This catamenia is characterized by frequent changes of presentations. The fetuses in breech presentation during this period have the same probability for breech and cephalic presentation at delivery.
During the 2nd period, lasting from the 25th to the 35th gestational week, the incidence of cephalic presentation increases, with a proportional decrease of breech presentation. The second menstruation is characterized by a higher than random probability that the fetal presentation during this period will likewise be present at the fourth dimension of delivery. The increment of this probability is gradual and identical for breech and cephalic presentations during this flow.
In the third flow, from the 36th gestational calendar week onward, the incidence of cephalic and breech presentations remain stable, i.e. breech presentation effectually 3–4% and cephalic presentation approximately 95%. In the full general population, incidence of breech presentation at preterm corresponds to the incidence of breech presentation when nascency occurs.[seven] [8] [9] [10] [eleven] [12] [13]
A breech presentation at delivery occurs when the fetus does not turn to a cephalic presentation.[14] This failure to change presentation tin result from endogenous and exogenous factors. Endogenous factors involve fetal inability to adequately move, whereas exogenous factors refer to insufficient intrauterine space available for fetal movements.[15]
Incidence of breech presentation amongst diseases and medical conditions with the incidence of breech presentation college than occurs in the full general population, shows that the probability of breech presentation is between 4% and 50%.[16] [17] [18] These data are related to:
- unmarried series of medical entities
- collections of serial for some particular medical entity
- information obtained from repeated observations under the same atmospheric condition
- series of ii concomitant medical conditions
Rates in various medical conditions [edit]
- Fetal entities:
- First twin 17–30%
- Second twin 28–39%
- Stillborn 26%
- Prader–Willi syndrome 50%, Werdnig–Hoffman syndrome 10%
- Smith–Lemli–Opitz syndrome 40%
- Fetal alcohol syndrome 40%
- Potter bibelot 36%
- Zellweger syndrome 27%
- Myotonic dystrophy 21%, 13 trisomy syndrome 12%
- eighteen trisomy syndrome 43%
- 21 trisomy syndrome five%
- de Lange syndrome 10%
- Anencephalus 6–eighteen%, Spina bifida 20–thirty%
- Congenital hydrocephalus 24–37%
- Osteogenesis imperfecta 33.iii%
- Amyoplasia 33.3%
- Achondrogenesis 33.3%
- Amelia 50%
- Craniosynostosis 8%
- Sacral agenesis 30.4%
- Arthrogriposis multiplex congenita 33.3
- Congenital dislocation of the hip 33.3%
- Hereditary sensory neuropathy type Three 25%
- Centronuclear myopathy xvi.7%
- Multiple pituitary hormone deficiency 50%
- Isolated pituitary hormone deficiency 20%
- Ectopic posterior pituitary gland 33.3%
- Built bilateral perisilvian syndrome 33.3
- Symmetric fetal growth restriction 40%
- Asymmetric fetal growth restriction xl%
- Nonimmune hydrops fetalis fifteen%
- Atresia ani 18.2%
- Microcephalus 15.four%
- Omphalocele 12.five%
- Prematurity 40%
- Placental and amniotic fluid entities:
- Amniotic sheet perpendicular to the placenta 50%
- Cornual–fundal implantation of the placenta thirty%
- Placenta previa 12.five%
- Oligohydramnios 17%
- Polyhydramnios 15.viii%
- Maternal entities:
- Uterus arcuatus 22.6%
- Uterus unicornuatus 33.3%
- Uterus bicornuatus 34.8%
- Uterus didelphys 30–41%
- Uterus septus 45.8%
- Leiomyoma uteri 9–20%
- Spinal cord injury 10%
- Carriers of Duchenne muscular dystrophy 17%
- Combination of two medical entities:
- First twin in uterus with ii bodies 14.29%
- 2nd twin in uterus with two bodies 18.52%.[18]
Also, women with previous Caesarean deliveries have a risk of breech presentation at term twice that of women with previous vaginal deliveries.[19]
The highest possible probability of breech presentation of 50% indicates that breech presentation is a event of random filling of the intrauterine space, with the aforementioned probability of breech and cephalic presentation in a longitudinally elongated uterus.[17]
Types [edit]
Types of breech depend on how the babe's legs are lying.[14]
- A frank breech (otherwise known as an extended breech) is where the baby's legs are up adjacent to its abdomen, with its knees direct and its feet adjacent to its ears. This is the nigh common type of breech.[20]
- A consummate breech (or flexed breech) is when the baby appears every bit though it is sitting crossed-legged with its legs bent at the hips and knees.[20]
- A footling breech is when one or both of the baby'southward feet are born first instead of the pelvis.[fourteen] This is more mutual in babies born prematurely or earlier their due date.[21]
- A kneeling breech is when the baby is born knees offset.[22]
In addition to the to a higher place, breech births in which the sacrum is the fetal denominator tin can be classified by the position of a fetus.[23] Thus sacro-anterior, sacro-transverse and sacro-posterior positions all exist, but left sacro-anterior is the most mutual presentation.[23] Sacro-inductive indicates an easier delivery compared to other forms.
Complications [edit]
Umbilical cord prolapse may occur, particularly in the complete, trivial, or kneeling breech.[24] This is acquired by the lowermost parts of the baby non completely filling the space of the dilated neck.[24] When the waters pause the amniotic sac, it is possible for the umbilical cord to driblet downwardly and become compressed.[24] This complication severely diminishes oxygen period to the infant, so the babe must exist delivered immediately (usually by Caesarean section[25]) and so that he or she tin breathe. If there is a delay in commitment, the brain can exist damaged. Among full-term, head-down babies, string prolapse is quite rare, occurring in 0.4 percent. Among frank breech babies the incidence is 0.5 percent,[24] amid complete breeches 5 percentage,[24] and among footling breeches xv percent.[24]
Head entrapment is acquired by the failure of the fetal head to negotiate the maternal midpelvis. At total term, the fetal bitrochanteric diameter (the altitude between the outer points of the hips) is about the same every bit the biparietal diameter (the transverse diameter of the skull)—merely put the size of the hips are the same as the size of the head. The relatively larger buttocks dilate the neck as effectively equally the caput does in the typical head-downward presentation. In dissimilarity, the relative head size of a preterm baby is greater than the fetal buttocks. If the babe is preterm, it may exist possible for the baby's body to emerge while the cervix has not dilated enough for the head to emerge.
Because the umbilical string—the baby's oxygen supply—is significantly compressed while the caput is in the pelvis during a breech birth, it is of import that the delivery of the aftercoming fetal head non be delayed. If the arm is extended alongside the head, delivery will not occur. If this occurs, the Løvset manoeuvre may exist employed, or the arm may be manually brought to a position in forepart of the chest.[26] The Løvset manoeuvre involves rotating the fetal torso by belongings the fetal pelvis. Twisting the trunk such that an arm trails behind the shoulder, it volition tend to cantankerous down over the face to a position where it can be reached past the obstetrician's finger, and brought to a position below the caput. A like rotation in the opposite direction is fabricated to deliver the other arm. In social club to present the smallest diameter (9.5 cm) to the pelvis, the baby's head must be flexed (chin to breast). If the head is in a deflexed position, the risk of entrapment is increased. Uterine contractions and maternal muscle tone encourage the head to flex.
Oxygen impecuniousness may occur from either cord prolapse or prolonged pinch of the cord during birth, as in caput entrapment. If oxygen deprivation is prolonged, information technology may cause permanent neurological damage (for case, cerebral palsy) or death. Information technology has been suggested that a fast vaginal delivery would mean the adventure of stopping baby's oxygen supply is reduced. However, there is not enough inquiry to show this and a quick commitment might cause more impairment to the infant than a bourgeois approach to the birth.[27]
Injury to the brain and skull may occur due to the rapid passage of the baby's head through the mother's pelvis. This causes rapid decompression of the baby's caput. In contrast, a baby going through labor in the head-downwards position ordinarily experiences gradual molding (temporary reshaping of the skull) over the grade of a few hours. This sudden compression and decompression in breech birth may crusade no bug at all, but it can injure the brain. This injury is more likely in preterm babies. The fetal head may be controlled by a special two-handed grip call the Mauriceau–Smellie–Veit maneuver or the elective application of forceps. This will be of value in controlling the rate of delivery of the head and reduce decompression. Related to potential head trauma, researchers have identified a relationship betwixt breech birth and autism.[28]
Squeezing the baby'southward abdomen can damage internal organs. Positioning the baby incorrectly while using forceps to evangelize the after coming head can damage the spine or spinal string. It is important for the birth bellboy to be knowledgeable, skilled, and experienced with all variations of breech birth.
Factors influencing safety [edit]
- Birth attendant'south skill (and experience with breech birth) – The skill of the medico or midwife and the number of breech births previously assisted is of crucial importance. Many of the dangers in vaginal nascence for breech babies come from mistakes made by nascence attendants. With the bulk of breech babies beingness delivered by cesarean department there is more risk that birth attendants will lose their skills in delivering breech babies and therefore increase the run a risk of harm to the baby during a vaginal delivery.[two] [29]
- Type of breech presentation – the frank breech has the almost favorable outcomes in vaginal birth, with many studies suggesting no divergence in consequence compared to head down babies.[thirty] (Some studies, all the same, notice that planned caesarean sections for all breech babies improve outcome. The divergence may rest in part on the skill of the doctors who delivered babies in unlike studies.) Complete breech presentation is the side by side most favorable position, but these babies sometimes shift and become niggling breeches during labour. Picayune and kneeling breeches have a higher risk of cord prolapse and head entrapment.[29]
- Parity – Parity refers to the number of times a woman has given birth before. If a adult female has given nativity vaginally, her pelvis has "proven" it is large enough to allow a infant of that babe's size to pass through information technology. Notwithstanding, a head-down baby's head often molds (shifts its shape to fit the maternal pelvis) so may present a smaller diameter than the same-size baby born breech.
- Fetal size in relation to maternal pelvic size – If the mother'southward pelvis is roomy and the babe is not large, this is favorable for vaginal breech delivery. However, prenatal estimates of the size of the baby and the size of the pelvis are unreliable.[29]
- Hyperextension of the fetal head – this tin can be evaluated with ultrasound. Less than 5% of breech babies have their heads in the "star-gazing" position, face looking straight upwards and the dorsum of the head resting confronting the dorsum of the neck. Caesarean delivery is absolutely necessary, because vaginal nascence with the baby'due south head in this position confers a loftier risk of spinal cord trauma and expiry.[29]
- Maturity of the baby – Premature babies appear to exist at higher chance of complications if delivered vaginally than if delivered past caesarean department.[29]
- Progress of labor – A spontaneous, commonly progressing, straightforward labor requiring no intervention is a favorable sign.[29]
- 2nd twins – If a first twin is born head down and the second twin is breech, the chances are skillful that the second twin can take a rubber breech birth.[31]
Management [edit]

Breech birth position seen on MRI
Equally in labour with a baby in a normal head-down position, uterine contractions typically occur at regular intervals and gradually the cervix begins to sparse and open.[32] In the more common breech presentations, the baby'due south bottom (rather than feet or knees) is what is first to descend through the maternal pelvis and emerge from the vagina.[24]
At the beginning of labour, the baby is mostly in an oblique position, facing either the right or left side. The baby'southward lesser is the same size in the term baby every bit the baby's head. Descent is thus as for the presenting fetal head and filibuster in descent is a cardinal sign of possible problems with the delivery of the head.
In order to begin the nascence, descent of podalic pole along with compaction and internal rotation needs to occur. This happens when the female parent'due south pelvic floor muscles cause the baby to turn so that information technology tin can be born with 1 hip straight in front of the other. At this betoken the baby is facing one of the mother'south inner thighs. Then, the shoulders follow the same path equally the hips did. At this fourth dimension the baby usually turns to face the mother's back. Next occurs external rotation, which is when the shoulders emerge as the babe'southward head enters the maternal pelvis. The combination of maternal muscle tone and uterine contractions cause the baby'southward caput to flex, mentum to chest. Then the back of the baby'south head emerges and finally the confront.
Due to the increased pressure during labour and nativity, it is normal for the baby'southward leading hip to be bruised and genitalia to be swollen. Babies who assumed the frank breech position in utero may continue to hold their legs in this position for some days after birth.[33]
Cesarean or vaginal commitment [edit]
When a babe is born bottom first there is more than hazard that the birth will not be direct forward and that the baby could be harmed.[3] For case, when the baby's head passes through the mother'southward pelvis the umbilical cord can be compressed which prevents delivery of oxygenated claret to the baby. Due to this and other risks, babies in breech position are often born by a planned caesarean section in developed countries.[2]
Caesarean department reduces the risk of harm or decease for the baby but does increase hazard of harm to the mother compared with a vaginal delivery.[ii] Information technology is best if the baby is in a head down position then that they tin can be born vaginally with less risk of harm to both mother and babe. The next section is looking at External cephalic version or ECV which is a method that can help the baby plow from a breech position to a head down position.
Vaginal birth of a breech baby has its risks only caesarean sections are non always bachelor or possible, a mother might go far in hospital at a tardily stage of her labour or may cull not to have a caesarean section. In these cases, information technology is important that the clinical skills needed to evangelize breech babies are not lost so that mothers and babies are as condom as possible.[2] Compared with developed countries, planned caesarean sections take non produced as practiced results in developing countries – information technology is suggested that this is due to more breech vaginal deliveries existence performed past experienced, skilled practitioners in these settings.[4]
Twin breech [edit]

Twin breech (vertex and non-vertex twins) [34]
In twin pregnancies, information technology is very mutual for one or both babies to exist in the breech position. Virtually oftentimes twin babies do non have the chance to turn around considering they are born prematurely. If both babies are in the breech position and the mother has gone into labour early on, a cesarean department may exist the best option. About 30–40% of twin pregnancies result in only ane baby beingness in the breech position. If this is the case, the babies tin can be built-in vaginally.[35] After the outset infant who is non in the breech position is delivered, the babe who is presented in the breech position may turn itself effectually, if this does not happen some other procedure may performed called the breech extraction. The breech extraction is the process that involves the obstetrician grabbing the second twin'south feet and pulling him/her into the nativity canal. This will help with delivering the second twin vaginally.[35] All the same, if the 2d twin is larger than the first, complications with delivering the 2nd twin vaginally may arise and a cesarean department should be performed. At times, the first twin (the twin closest to the birth canal) can be in the breech position with the 2nd twin being in the cephalic position (vertical). When this occurs, risks of complications are higher than normal. In item, a serious complication known as Locked twins. This is when both babies interlock their chins during labour. When this happens a cesarean section should be performed immediately.
Turning the baby [edit]
Turning the baby, technically known as external cephalic version (ECV), is when the baby is turned by gently pressing the mother'southward belly to push the babe from a bottom start position, to a head first position.[3] ECV does non e'er work, but it does improve the mother's chances of giving nativity to her baby vaginally and avoiding a cesarean department. The World Wellness Organization recommends that women should have a planned cesarean department only if an ECV has been tried and did not piece of work.[four]
Women who have an ECV when they are 36–40 weeks pregnant are more likely to have a vaginal delivery and less likely to have a cesarean section than those who practice not accept an ECV.[27] Turning the babe before this time makes a caput first nativity more probable but ECV earlier the due appointment can increase the risk of early or premature birth which tin crusade problems to the infant.[3]
There are treatments that can be used which might touch the success of an ECV. Drugs chosen beta-stimulant tocolytics help the woman'due south muscles to relax and so that the pressure during the ECV does not have to exist and so bully. Giving the woman these drugs earlier the ECV improves the chances of her having a vaginal commitment because the babe is more probable to plough and stay caput down.[36] Other treatments such equally using sound, pain relief drugs such as epidural, increasing the fluid effectually the baby and increasing the corporeality of fluids to the adult female before the ECV could all outcome its success but there is not plenty enquiry to make this clear.[36]
Turning techniques mothers can practise at dwelling are referred to as "spontaneous cephalic version" (SCV), this is when the babe can turn without any medical aid.[37] Some of these techniques include: a knee-to-chest position, the breech tilt, and moxibustion, these tin can be performed subsequently the female parent is 34 weeks significant.[ citation needed ] There is limited evidence that these techniques have whatever effect.[ citation needed ]
Notable cases [edit]
- Chesa Boudin[38]
- Jordan Brady[39]
- Becky Garrison[40]
- Billy Joel[41]
- Jerry Lee Lewis[42]
- Bret Michaels[43]
- Nero[44]
- Tatum O'Neal[45]
- David Shields[46]
- Frank Sinatra[47]
- Wilhelm Ii, German Emperor[48]
- Pedro Zamora[49]
- Frank Zappa[50]
See as well [edit]
- Asynclitic birth, another abnormal nativity position
References [edit]
- ^ "Breech nascence: MedlinePlus Medical Encyclopedia". medlineplus.gov . Retrieved 2020-ten-29 .
- ^ a b c d eastward f chiliad Hofmeyr, GJ; Hannah, M; Lawrie, TA (21 July 2015). "Planned caesarean department for term breech delivery". The Cochrane Database of Systematic Reviews. vii (7): CD000166. doi:10.1002/14651858.CD000166.pub2. PMC6505736. PMID 26196961.
- ^ a b c d Hutton, EK; Hofmeyr, GJ; Dowswell, T (29 July 2015). "External cephalic version for breech presentation before term". The Cochrane Database of Systematic Reviews. seven (7): CD000084. doi:x.1002/14651858.CD000084.pub3. PMID 26222245.
- ^ a b c Conde-Agudelo, A. "Planned caesarean section for term breech delivery: RHL commentary (concluding revised: 8 September 2003)". The WHO Reproductive Wellness Library. Geneva: Globe Health Organization. Archived from the original on March ane, 2016. Retrieved xix February 2016.
- ^ "Infant's Death Sparks A Heated Debate Effectually The "Free Nascence" Move". BuzzFeed News . Retrieved 2020-02-22 .
- ^ "Your baby in the birth canal: MedlinePlus Medical Encyclopedia". medlineplus.gov . Retrieved 2020-10-29 .
- ^ Miller EC, Kouam L (1981). "Frequency of breech presentation during pregnancy and on full term". Zentralbl Gynakol. 103: 105–109.
- ^ Colina L (2008). "Prevalence of Breech Presentation by Gestational Historic period". American Journal of Perinatology. 7 (1): 92–93. doi:10.1055/due south-2007-999455. PMID 2403797.
- ^ Hughey MJ (1985). "Fetal position during pregnancy". Am J Obstet Gynecol. 153 (8): 885–886. doi:10.1016/s0002-9378(85)80276-3. PMID 3907357.
- ^ Sørensen, T; Hasch, Eastward; Lange, AP (1979). "Fetal presentation during pregnancy". Lancet. 2 (8140): 477. doi:x.1016/s0140-6736(79)91536-8. PMID 89542. S2CID 13263722.
- ^ Tadmor OP, Rabinowitz R, Alon L, Mostoslavky V, Aboulafia Y. Can breech presentation at birth be predicted from ultrasound examination during the second or third trimester?" Int J Gynaecol Obstet 1994;46:11–xiv.
- ^ Boos, R; Hendrik, HJ; Schmidt, W (1987). "Beliefs of fetal position in the second half of pregnancy in labor with breech and vertex presentations". Geburtshilfe Frauenheilkd. 47 (v): 341–345. doi:10.1055/due south-2008-1035833. PMID 3301520.
- ^ Witkop, CT; Zhang, J; Sunday, West; Troendle, J (2008). "Natural history of fetal position during pregnancy and risk of nonvertex commitment". Obstet Gynecol. 111 (four): 875–880. doi:x.1097/aog.0b013e318168576d. PMID 18378746. S2CID 23118359.
- ^ a b c "Breech - series—Types of breech presentation: MedlinePlus Medical Encyclopedia". medlineplus.gov . Retrieved 2020-x-29 .
- ^ Sekulić S, Zarkov Thou, Slankamenac P, Bozić Chiliad, Vejnović T, Novakov-Mikić A (2009). "Decreased expression of the righting reflex and locomotor movements in breech-presenting newborns in the first days of life". Early Human Development. 85 (iv): 263–6. doi:10.1016/j.earlhumdev.2008.11.001. PMID 19028029.
- ^ Braun FH, Jones KL, Smith DW (1975). "Breech presentation as an indicator of fetal aberration". J Pediatr. 86 (3): 419–21. doi:10.1016/s0022-3476(75)80977-2. PMID 1113232.
- ^ a b Sekulić SR, Mikov A, Petrović DS (2010). "Probability of breech presentation and its significance". J Matern Fetal Neonatal Med. 23 (10): 1160–4. doi:ten.3109/14767051003677996. PMID 20230320. S2CID 5984573.
- ^ a b Sekulić SR, Petrović DS, Runić R, Williams Thousand, Vejnović TR. Does a probability of breech presentation of more than 50% exist among diseases and medical weather? Twin Res Hum Genet. 2007; ten:649–54.
- ^ Vendittelli F., Rivière O., Crenn-Hébert C., Rozan G. A., Maria B., Jacquetin B. (2008). "Is a breech presentation at term more frequent in women with a history of cesarean delivery?". American Journal of Obstetrics and Gynecology. 198 (5): 521.e1–6. doi:ten.1016/j.ajog.2007.11.009. PMID 18241817.
{{cite periodical}}: CS1 maint: multiple names: authors listing (link) - ^ a b "Agreement fetal presentation before birth". Mayo Dispensary . Retrieved 2020-x-29 .
- ^ Tidy, C. "Breech Presentations (concluding revised xi/03/2013)". Retrieved 2 March 2016.
- ^ Ottawa, Hospital (July 5, 2021). "Vaginal Breech Nascence Plan". www.ottawahospital.on.ca.
- ^ a b Konar, Hiralal (2014). Dc dutta's textbook of obstetrics (7th ed.). [Due south.l.]: Mcgraw-Loma. p. 376. ISBN978-93-5152-067-2.
- ^ a b c d e f one thousand Payne, J. "Prolapsed Cord. Pregnancy complications from prolapsed cord". Patient info . Retrieved 22 April 2016.
- ^ "Umbilical String Prolapse" (PDF). Regal College of Obstetricians and Gynaecologists. November 2014. Retrieved 22 April 2016.
- ^ Tidy, C. "Breech Presentations". Patient . Retrieved 22 April 2016.
- ^ a b Hofmeyr, GJ; Kulier, R; West, HM (21 July 2015). "Expedited versus conservative approaches for vaginal delivery in breech presentation". The Cochrane Database of Systematic Reviews. 7 (7): CD000082. doi:10.1002/14651858.CD000082.pub3. PMC6505640. PMID 26197303.
- ^ Bilder Deborah, Pinborough-Zimmerman Judith, Miller Judith, McMahon William (2009). "Prenatal, Perinatal, and Neonatal Factors Associated With Autism Spectrum Disorders". Pediatrics. 123 (5): 1293–1300. doi:ten.1542/peds.2008-0927. PMID 19403494. S2CID 36884801.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b c d eastward f Kotaska, A; Menticoglou, S; Gagnon, R; Farine, D; Basso, M; Bos, H; Delisle, MF; Grabowska, Chiliad; Hudon, L; Mundle, West; Irish potato-Kaulbeck, L; Ouellet, A; Pressey, T; Roggensack, A; Maternal Fetal Medicine, Committee; Social club of Obstetricians and Gynaecologists of, Canada (June 2009). "Vaginal commitment of breech presentation". Journal of Obstetrics and Gynaecology Canada. 31 (6): 557–66, 567–78. doi:ten.1016/s1701-2163(16)34221-9. PMID 19646324.
- ^ Datta, Sanjay (2004-01-09). Anesthetic and Obstetric Management of High-Risk Pregnancy. Springer Scientific discipline & Business Media. ISBN9780387004433.
- ^ Kotaska A, Menticoglou S, Farine D; et al. (Jun 2009). "Vaginal commitment of breech presentation". J Obstet Gynaecol Tin. 31 (6): 557–66, 567–78. doi:10.1016/s1701-2163(16)34221-9. PMID 19646324.
{{cite journal}}: CS1 maint: multiple names: authors listing (link) (reference is for entire section) - ^ "Offset stage". StratOG. Royal College of Obstetricians and Gynaecologists. 2016. Archived from the original on 2016-04-27. Retrieved 22 Apr 2016.
- ^ McClain, L (2016). "Volition my newborn be different? – Better Birth Blog". Better Birth Blog . Retrieved xviii March 2016.
- ^ "Twin Breech".
- ^ a b "Delivery of Breech 2nd Twin". Healthline . Retrieved 2016-05-17 .
- ^ a b Cluver, C; Gyte, GM; Sinclair, Thousand; Dowswell, T; Hofmeyr, GJ (nine February 2015). "Interventions for helping to plough term breech babies to head first presentation when using external cephalic version". The Cochrane Database of Systematic Reviews. 2 (2): CD000184. doi:10.1002/14651858.CD000184.pub4. hdl:10019.ane/104301. PMID 25674710.
- ^ "How tin can I plough my breech babe naturally?". BabyCentre . Retrieved 2016-05-sixteen .
- ^ Wilgoren, Jodi (nine December 2002). "From a Radical Background, A Rhodes Scholar Emerges". New York Times . Retrieved 3 February 2015.
- ^ "'I Am Comic' Director Hashemite kingdom of jordan Brady on Spit Takes and the Downside of Supportive Audiences". Interview. The Sense of humour Code. 15 March 2012. Retrieved 2 February 2015.
- ^ Garrison, Becky (1 Jan 2008). The New Atheist Crusaders and Their Unholy Grail: The Misguided Quest to Destroy Your Faith. Thomas Nelson Inc. p. 133. ISBN9781418574550.
- ^ Andrew Goldman (26 May 2013). "Baton Joel on not working, not giving up drinking and not caring what Elton John says virtually whatsoever of it". New York Times Magazine. p. 34. Retrieved 2 February 2015. Joel attributes the need for double hip replacement surgery to "probably existence born with dysplasia." He explains that he was a breech baby and that forceps may have displaced his hips.
- ^ McKennain, Mike (26 February 2010). "Bang-up balls of wax". Retrieved 3 February 2015. Allegedly said, "I was built-in feet get-go, and I've been jumpin' ever since."
- ^ Ellis, Christine (15 April 2012). "Music for your soul". His website. Bret Michaels. Archived from the original on 22 Apr 2016. Retrieved 3 February 2015.
- ^ Geffcken, Katherine A.; Dickison, Sheila Kathryn; Hallett, Judith P. (2000). Rome and Her Monuments: Essays on the City and Literature of Rome in Award of Katherine A. Geffcken. Bolchazy-Carducci Publishers. p. 496. ISBN9780865164574.
- ^ O'Neal, Tatum (4 October 2005). A Paper Life . HarperCollins. pp. 14. ISBN9780060751029.
i was born breech.
- ^ Shields, David (2009). The Thing near Life Is That One Day Yous'll Be Dead. Random House LLC. p. 4. ISBN9780307387967.
- ^ Santopietro, Tom (x Nov 2009). Sinatra in Hollywood. Macmillan. p. 12. ISBN9781429964746.
- ^ Putnam, William L. (2001). The Kaiser's merchant ships in Globe War I. p. 33.
- ^ Winick, Judd (2000). Pedro and Me: Friendship, Loss, and What I Learned. Henry Holt & Co. pp. 33–36.
- ^ Miles, Barry (2004). Zappa . Grove Press. pp. 5.
was born breech.
External links [edit]
- Breech birth controversies in Great Britain
- GLOWM video demonstrating vaginal breech delivery techniques
Source: https://en.wikipedia.org/wiki/Breech_birth
0 Response to "Why Is a Baby in Breech Uncomfortable to Carry?"
Post a Comment